|
by Cindy Abole
Public Relations
Imagine it’s fourth down and the ball is within kicking distance
of the field goal. The coach assesses the situation and calls for the
team’s specialty group—the team’s field goal kicker and unit, to do
their job at the right time during the game.
The same concept applies to specialty care among critically ill patients.
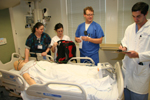 Medical
Emergency Team (MET) respiratory therapist Mindy Repphen-Harvey, from
left, and team nurses Alisha Mangaro and Seth Long respond to a call on
a simulated patient at the MUSC Health Care Simulation Center in the
College of Nursing. Pulmonology fellow, Dr. David Pucci, who is part of
MET, reviews training details. Medical
Emergency Team (MET) respiratory therapist Mindy Repphen-Harvey, from
left, and team nurses Alisha Mangaro and Seth Long respond to a call on
a simulated patient at the MUSC Health Care Simulation Center in the
College of Nursing. Pulmonology fellow, Dr. David Pucci, who is part of
MET, reviews training details.
For
almost two years, MUSC has managed a specialty clinical team that
brings critical care expertise to the bedside anywhere in the hospital.
MUSC’s Medical Emergency Team (MET) program, which began in January
2007, provides a level of specialized care to patients with clinical
instability or a worsening condition. The service is available to adult
and pediatric patients at ART, MUSC hospital and the Children’s
Hospital. The concept is to provide an immediately available,
interdisciplinary, specialized team approach to patients with
deteriorating health status and thus improve the quality of in-patient
care.
MET teams consist of a critical care nurse, respiratory therapist and
intensive care (ICU) physician who work with each other and the
patient’s primary team in stabilizing a patient and contributing to
their overall care.
“Nurses on the floor really need these critical care nurses and
specialists to help them care for critically ill patients,” said Sheila
Scarbrough, R.N., critical interventions manager, quality and outcomes
in the medical director’s office and MET coordinator. Scarbrough works
with Dee Ford, M.D., assistant professor of medicine, Division of
Pulmonary and Critical Care Medicine who works in the Medical ICU
(MICU) and Digestive Diseases ICU (DDICU). “Floor staff are
often not trained to care for critically ill patients and additionally
have multiple competing demands on their time. This program activates a
system to bring critical care resources immediately to a patient’s
beside and activates the Admit Transfer Center to begin the process of
procuring an ICU bed in case this patient requires transfer.”
Scarbrough added that about 50 percent of MET’s are transferred into an
ICU.
MET was developed from criteria documented in medical literature
associated with patients who are at increased risk for a
cardiopulmonary arrest. The physician-led program began as a pilot
program in the main hospital’s 6E, 7E and 8E and has been offered 24/7
since October 2007.
MET also meets recognition and response criteria relating to a
patient’s condition under the Joint Commission’s 2008 National Patient
Safety Goals. In January 2007, MUHA established Policy C-149 “Medical
Emergency Teams.” The concept involves a team intervention approach to
providing specialized critical care to patients prior to an acute
crisis such as cardiopulmonary arrest.
Medical staff assesses at-risk patients for changes in blood pressure,
heart rate, breathing, mental status and other criteria. Medical or
nursing staff can activate the MET via the paging operator
(792-3333). The MET staff member will confer with the patient’s
attending physician or their designee to outline a treatment plan. The
MET physician also will document findings/actions in the progress
notes.
Cindy Hough, R.N., 6E nurse manager, is an advocate for MET among her
staff and throughout the medical center. Hough and her team care for
some of the hospital’s most seriously ill patients—transplant patients.
“MET is a positive approach to patient-centered care,” said Hough, who
has more than 12 years experience as a transplant nurse. “It provides
the needed resources at the right time and saves nursing time while
bolstering patient safety.”
8E Medical Acute Care nurse manager Helena Walo, R.N., echoes that
level of support for MET. Walo believes MET is not meant as a
judgmental reflection on staffing care but empowers nurses to make
decisions that provide the highest level of patient care.
“MUSC leadership has been great to support this as an important
instrument to improve patient outcomes,” said Walo. “It provides a good
opportunity for an ICU-level team to partner with primary care
physicians and staff in following a patient’s care. Walo heads the
medical center’s MET watch pilot program on 8E that provides non-ICU,
inpatient nurses with specific guidelines to identify patients at high
risk for needing MET team intervention.
An ongoing challenge according to Scarbrough is getting physicians and
staff to call for MET at the first sign of a patients' decline.
In 2009, additional MET information will be related to patients and
families via MUSC’s GetWell Network. In the meantime, Scarbrough, Ford
and staff will be collecting data and evaluating numbers for trends
while looking for opportunities for improvement. So far, MUSC has
increased their MET call rate from less than three calls to greater
than 10 calls per 1,000 discharges. Hospitals with higher MET call
rates demonstrate better patient outcomes.
“We want families and visitors to be more aware of what MET is and that
it is a level of expertise that we provide throughout the hospital
system. It is a benefit for all patients of MUSC that we have this team
that’s there to take care of their loved one throughout their hospital
stay,” Scarbrough said.
Friday, Jan. 9, 2009
|



