|
by Maggie Mullen
Public Relations
MUSC researchers have become national leaders with a new neurosurgical
procedure. The teamwork among Ziad Nahas, M.D., Istvan Takacs, M.D.,
and Scott Reeves, M.D., helped to pioneer bilateral epidural prefrontal
cortical stimulation (EpCS) in the brain, which proved generally safe
and provided significant improvement of depressive symptoms.
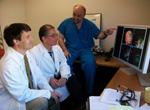 Dr.
Istvan Takacs points out the computer image of a bilateral epidural
prefrontal cortical stimulation (EpCS) in the brain to Drs. Ziad Nahas,
center, and Scott Reeves. This work was funded by the National Alliance
of Research in Schizophrenia and Affective Disorders, while a local
resource, General Clinical Research Center, was critical in covering
perioperative costs. The devices were donated by Medtronic Inc. Dr.
Istvan Takacs points out the computer image of a bilateral epidural
prefrontal cortical stimulation (EpCS) in the brain to Drs. Ziad Nahas,
center, and Scott Reeves. This work was funded by the National Alliance
of Research in Schizophrenia and Affective Disorders, while a local
resource, General Clinical Research Center, was critical in covering
perioperative costs. The devices were donated by Medtronic Inc.
For information, call 876-5142.
“Cortical stimulation is
reversible, non-destructive and potentially safer than other forms of
invasive brain stimulation since the stimulating paddles do not come in
direct contact with the brain,” said Nahas, associate professor of
Psychiatry, Physiology and Neuroscience and director of MUSC's Mood
Disorders Program. “These preliminary results are encouraging but not
definitive. Now that we have a proof of concept, we should aim at
studying bilateral EpCS in larger placebo-controlled studies.”
Pushing this idea for four years, Nahas is the principal investigator
who collaborated with both Takacs and Reeves. The study consisted of
implanting EpCS into five patients over the anterior frontal poles and
the lateral prefrontal cortex. These areas are important in regulating
mood and social behavior. Paddle leads were then connected to small
generators surgically implanted into the chest area. Patients were
followed over a seven-month period as the devices periodically
delivered low electrical charges, which were individualized for each,
and then were evaluated using standard clinical ratings. Only patients
who have tried several medications and treatments without success were
included in the study.
“The more sophisticated functions are on the surface of the brain,”
said Takacs. “We are trying to change the climate within the prefrontal
cortex so it could exert more adaptive governance of deeper brain
regions,” he said.
The average improvement was between 50 to 60 percent based on varying measures. Three patients reached remission.
“This groundbreaking pilot study emphasizes the synergism that can
occur when multiple departments and researchers come together to
develop possible solutions to complex clinical problems, such as
refractory depression,” said Reeves.
Nahas’ immediate team involved Berry Anderson, Ph.D., and Ashley Arana.
Other contributors were Mark George, M.D., Distinguished University
Professor, Department of Psychiatry and Behavioral Science, and Jeff
Borckardt, Ph.D., associate professor, Department of Psychiatry and
Behavioral Science. The departments of Psychiatry and Behavioral
Science, Neurosurgery, and Anesthesia and Perioperative Medicine
collaborated to make this possible.
For more information, call 876-5142.
Friday, Nov. 27, 2009
|



