|
|
|

|
New test reduces time, improves quality of imaging
|
by Dawn Brazell
Public Relations
The first advantage a cardiac patient is likely to notice is that the
test takes less time—one hour as compared to four. The doctors will
notice the improved quality in imaging as well.
Leonie Gordon, M.D., Marques Bradshaw, M.D., and Kenneth M. Spicer,
M.D., Ph.D., and their cardiology colleagues, will be celebrating both
and looking for ways to expand the research opportunities provided by a
new type of advanced imaging system at MUSC. The new procedure, called
rubidium PET/CT myocardial perfusion scanning, combines Positron
Emission Tomography (PET) with Computed Tomography (CT). In less than
an hour, this noninvasive imaging technology provides quality images
that can help physicians better diagnose and treat coronary artery
disease.
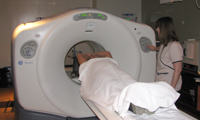 Melissa Dutton, a
nuclear medicine technologist, likes that the rubidium PET/CT scanner
shortens the testing time for patients. Melissa Dutton, a
nuclear medicine technologist, likes that the rubidium PET/CT scanner
shortens the testing time for patients.
One of the most promising features of the technology is that it
delivers more accurate imaging for patients with a body mass index
(BMI) of more than 28, for patients weighing 250 pounds or more, or for
people who are stocky or large-breasted.
A major advantage is that rubidium PET/CT myocardial perfusion imaging
gives the patient a significantly reduced radiation dose, approximately
one third of the exposure received from a standard nuclear medicine
cardiac perfusion scan.
Spicer said the hospital began rubidium myocardial perfusion imaging in
October and MUSC is the one of about a dozen sites in the Southeast to
be using this technology.“It’s a much less extensive procedure because
the radioisotope has a very short half life—about a minute—half of it
goes away every minute. We image very quickly, and can wait five to 10
minutes and repeat the procedure. With normal nuclear medicine imaging
of the heart muscle, we use technetium with a six hour half life.”
Having a procedure with improved specificity is extremely helpful as
well, he said. Large body size can impair the ability of photons, the
particles of energy that come from the radioactive tracer, to register
correctly on the imaging camera. PET/CT scanners can minimize this
problem. Further, the higher energy level of the radioactive photons
emitted from rubidium move through tissue more freely, thus providing
better, more accurate imaging, he said.
Another benefit is patients don’t have to remain still as long, so
there is less blurring of the images from motion. This newer imaging
procedure is just as safe and is not more expensive, two factors
important in its effectiveness in treating patients, said Spicer.
 Dr. Kenneth Spicer Dr. Kenneth Spicer
“One of the greatest frustrations for nuclear medicine physicians and
cardiologists occurs when they are confronted with an ambiguous scan,”
said Spicer, explaining this too often is the case with patients with a
larger body mass. “The ambiguous scan can be caused by excessive tissue
scattering of photons, by motion or be a real lesion in the coronary
artery that is potentially life threatening to the patient. We have to
tell the referring physician that we’re not sure.”
Patients may request the newer imaging procedure and should if they
have a larger body mass. “Clearly this would be a better procedure for
them.”
PET scanning acquires images by detecting the radioactive tracer
rubidium. Special cameras can detect photons being produced in the
blood stream by this radiopharmaceutical and compute a map of the
way blood is being distributed to heart tissue. The CT part of the
combined imaging system uses rotating X-ray beams to pinpoint normal
and abnormal cardiac blood flow. The combined system measures that flow
in precise, numerical terms, which is ultimately what is required for
optimal treatment, he said.
Spicer said doctors can more accurately measure heart muscle activity
with PET scanning than they can with standard nuclear medicine
procedures. “That allows us to image actual metabolic activity of the
heart muscle cells, which is important in terms of improving our
sensitivity for diagnosing serious disease processes.”
Early detection and treatment of incomplete or small partial blockages
seen with other, anatomic imaging procedures also has the potential to
protect heart muscle, but this can be invasive and expensive, he said.
Rubidium PET/CT scans optimally depict not only whether a coronary
artery blockage is impairing blood flow to the heart muscle, but also
the extent of the decreased flow.
That ability translates into exciting research applications, Spicer
said.
When combined with another tracer called FDG, which assesses sugar
molecules the heart burns as a fuel, PET/CT produces a clear picture of
viable areas of heart muscle and differentiates them from those that
are scarred, or even from viable muscle cells that are temporarily
stunned. This distinction can help doctors decide which treatments
would be the most effective.
This type of scanning, known as Metabolic Imaging, also takes health
professionals one step closer to being able to make earlier diagnoses.
There is a progression or stairway of changes that occur as a disease
process evolves, Spicer said. “When something goes wrong, it usually
produces genetic code changes within a cell. It could be a virus that
came in. It could be a chemical shock or even physical injury. But
there’s been something that changes the metabolism of the cell. If
you’re going to be the most sensitive, you want to catch the changes
that occur at that point. We’re not quite that good yet.”
The next step in disease progression is that the biochemical
alterations result in changes in the function of the injured cell. For
the heart this could mean EKG changes, or heart wall motion decreases.
Finally, the shapes of the cell or groups of cells change, he said.
“Typically in radiology we’re imaging the end of the chain—the
shape—when the muscle cells die and the heart wall becomes thin or
scarred, to an extent that is big enough to see it. That’s obviously
very helpful, but it’s not nearly as sensitive as it needs to be. In
Metabolic Imaging, we can step down these stairs getting closer and
closer to the original event where things started going wrong. That’s
where the real forte of PET/CT imaging is.”
Friday, Dec. 15, 2010
|
|
|




