|
By Dawn
Brazell
Public Relations
Cynde Brown
sits tall, flipping back a strand
of auburn hair.
"There's no
shame to my game," she said. She
just described her recent double
mastectomy and reconstruction
involving one of the latest
plastic surgery techniques called
DIEP or deep inferior epigastric
artery perforator flap. The
procedure uses the fat and skin
from the lower abdominal area to
reconstruct the breasts by
connecting the blood vessels from
the abdomen to the blood vessels
in the chest wall.
She pats her
flat stomach. "You can still wear
the sexy stuff. You don't let what
the world thinks of you define
your own image. Your breasts do
not define you. You are defined by
yourself – your personality, your
soul. Take control of your life.
Don't sit there and wait and be a
victim. If you can prevent it,
take the most steps you can to
prevent – whatever it may be."
Spoken as the
spunky survivor that she is,
Brown's first troubles started at
age 6 when she was diagnosed with
autoimmune hepatitis. As a result
her liver failed, and she received
a liver transplant at MUSC at age
31 in 1998, just a year after
having lost her mother. Still
reeling from her losses, Brown
hoped that other than her routine
checkups, she was done with her
surgeries.
 Cynde Brown's
daughter, shown in the photo in
her hand, is one of her main
motivators in getting the
information she needs about all
the latest treatments of breast
cancer to make the right
decisions. Cynde Brown's
daughter, shown in the photo in
her hand, is one of her main
motivators in getting the
information she needs about all
the latest treatments of breast
cancer to make the right
decisions.
Unfortunately
in 2005, her sister was diagnosed
with metastatic breast cancer.
Brown eventually got her sister's
pathology reports and sought
genetic testing in 2008, finding
that she also tested positive for
the BRCA 1 mutation. Harmful
mutations in these genes produce a
hereditary breast-ovarian cancer
syndrome. As a preventative
measure, Brown had both ovaries
removed.
In 2010 an MRI
revealed she had two masses in her
left breast so she decided, given
her BRCA 1 status and being immune
suppressed for life as a
transplant patient, to opt for a
double mastectomy with immediate
reconstruction done on the same
day at MUSC. The masses turned out
to be benign, but Brown said it
was the right decision because
having the gene meant it was only
a matter of time.
Dr. Dennis
Schimpf, left, Department of
Surgery, performs a breast
reconstruction. The Division of
Plastic Surgery completes more
than 400 breast reconstruction
cases per year. Microvascular
breast reconstruction cases
(such as DIEP) comprise more
than 100 of the breast
reconstructions that are
completed each year. For
information on breast
reconstruction, visit http://www.breastreconstructionofcharleston.com.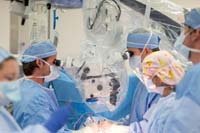
There was a
time not so long ago when Brown
wouldn't have had so many options.
With advances
in genetic testing and
reconstruction procedures,
including the availability of 3-D
nipple tattooing, breast cancer
survivors can take more proactive
stances. Making those choices
helps her feel empowered, a
critical element for someone who
has spent as much time in
hospitals as she has, she said.
She believes in doing her research
and is intent on keeping a good
attitude.
"It comes from
my mother, and it comes from
faith. Just knowing that I can't
change what's going to happen, the
best thing I can do is deal with
it the best way that I can. Who
wants to be around someone who's
complaining all the time? I don't.
Be happy. Be glad for every day
you have."
Destination
Center
One advantage that made Brown
decide to get her mastectomy,
other than being strongly
encouraged by her various doctors,
was that she could get the
mastectomy and reconstruction done
in the same day. That was a deal
maker for her. David Cole, M.D.,
Rose Professor and chairman of the
Department of Surgery, handled her
double mastectomy and plastic
surgeon Dennis Schimpf, M.D., did
her DIEP reconstruction.
Schimpf said
the goal is to make life simpler
for women with breast cancer, so
Hollings Cancer Center (HCC) tries
to offer a complete package to
patients. He's pleased how MUSC's
HCC, which holds a National Cancer
Institute (NCI) designation, is
growing to be a destination center
for breast reconstruction.
HCC has a
high-risk breast program that
includes genetic testing and
counseling and a comprehensive
array of surgical options. The
Division of Plastic Surgery offers
the entire range of breast
reconstruction procedures from
traditional, implant-based
reconstruction, to the most
advanced perforator-based
(DIEP) forms of
reconstruction that are available
today, he said.
"We have a
tremendous amount of experience in
breast reconstruction secondary to
our large volume of cases. We
also tend to do the more difficult
cases on the more high risk or
difficult patients and often times
are the last hope for women who
have had difficulties with
previous reconstructions or who
have been turned down by other
centers."
Schimpf helped
bring Renee Maschinot onto the
team. The medical tattoo artist
travels from Florida to MUSC every
other month to offer areola and
3-D nipple tattoos.
"Plastic
surgery offers the opportunity to
impact both the appearance and the
function of patients by operating
on all areas of the
body in patients of all ages.
As a result of being a part of the
only NCI cancer center in South
Carolina, we can offer patients
access to the highest level of
cancer care, breast reconstruction
and support services, such as
nutrition, physical therapy,
counseling and survivorship
groups."
The approach is
to have a
multidisciplinary team
working together to treat the
physical and emotional needs of
each patient.
"We treat each
patient as an individual and make
recommendations and schedule
appointments to accommodate each
patient's comfort and convenience.
Our program is designed to
centralize all outpatient breast
cancer/reconstruction services in
one location so that patients do
not have to travel to multiple
locations for appointments. We
strive to anticipate and address
the needs of our patients."
Being
Well-Informed
For Brown, that is crucial. She
has to travel 150 miles from
Latta, outside of Florence, to get
here. Brown said her health is
worth the drive, but she's glad to
combine as many appointments as
she can when she comes.
Having had so
many medical issues, she has
learned how to best navigate the
health care system. She advises
patients to engage their health
care providers and do their
research on all the options now
available, especially for women
with or at high risk for breast
cancer.
"This will
ensure that they have all of the
knowledge necessary to make a
well- informed decision."
Brown holds up a picture of her
5-year-old daughter – one of her
motivations in being as
well-informed as she could. She
wants to be around to see her grow
up. Sometimes people ask her if
she made the right decision to
have her breasts removed before
cancer struck.
"I think I did
the right thing. I feel very
confident in my decision. It is a
drastic step. But with that
genetic testing, it is not a
matter of if you're going to get
breast cancer. I know I'm going
to. It's a matter of when. I chose
not to wait for the when."
Studying her options for
reconstruction was empowering as
well.
"I was tickled
by the fact it was going to be a
breast reduction. I can wear cute
bras and cute shirts. I am going
to have a tummy tuck. I'm like,
'Lord, I haven't had a flat belly
in years.'"
Brown chose the
DIEP flap because it used her own
tissue and will respond to her
natural weight gain and losses. If
she couldn't have it done, she's
not sure if she would still have
opted to have the double
mastectomy.
Despite all her
brave decisions, she knows there
remains a small chance she still
can get cancer. She relies on her
strong Christian faith. Her goal
is to show her daughter how to
look at all the different options
there are in life when a challenge
arises and choose the path of not
being a victim, she said.
"If I get
breast cancer now, then so be it.
That is just my destiny. I have
done everything I physically can
to prevent it. If I get it, then
it's, 'OK, what are we going to do
now?' What do you want to do and
when can you do it?"
Breast
Reconstruction
As a destination center for breast
reconstruction, MUSC is offering
the latest in services and
procedures, including the DIEP
flap breast reconstruction (deep
inferior epigastric perforator
flap). It is one of the most
advanced forms of breast
reconstruction offered that
relocates excess tissue from one
area of the body. Donor sites for
flap reconstruction often include
the abdomen, buttocks, thigh, or
back. The decision as to which
type of flap to have is based on
many factors including: the amount
of tissue available at the donor
site and the breast size desired
by the patient, placement of
scars, and the patient's surgical
history.
Visit http://www.breastreconstructionofcharleston.com for
information on MUSC's Advanced
Breast Reconstuction Program.
Renee
Maschinot's story as an areola
and 3-D nipple tattoo artist.
|



 Cynde Brown's
daughter, shown in the photo in
her hand, is one of her main
motivators in getting the
information she needs about all
the latest treatments of breast
cancer to make the right
decisions.
Cynde Brown's
daughter, shown in the photo in
her hand, is one of her main
motivators in getting the
information she needs about all
the latest treatments of breast
cancer to make the right
decisions. 