|
|
|

|
Islet cell transplant offers promising lifeline
|
by Dawn Brazell
Public Relations
Thrilled that MUSC’s pioneering efforts led to the milestone of the
50th islet cell transplant Jan. 31, David Adams’ mission is to end the
suffering of patients with chronic pancreatitis.
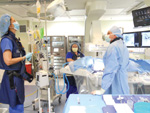 Interventional
radiologist Renan Uflacker (right), registered nurses Monica Mallory,
center, and Hedy Fagan oversee islet cells being infused into a
patient’s liver. Watch a Video:
visit http://tinyurl.com/6xb2z4v Interventional
radiologist Renan Uflacker (right), registered nurses Monica Mallory,
center, and Hedy Fagan oversee islet cells being infused into a
patient’s liver. Watch a Video:
visit http://tinyurl.com/6xb2z4v
MUSC holds the distinction of being the second busiest autologous islet
cell transplant center in the country, behind the University of
Minnesota, which started doing the procedure in the 1970s. MUSC, the
only place in the state to offer the procedure, treated its first
patient March 2009, and performs about 25 cases a year to treat chronic
pancreatitis. The condition afflicts thousands of patients and is
characterized by debilitating pain and suffering that frequently is
unresponsive to traditional medical and surgical treatments, said
Adams, M.D.
“Chronic pancreatitis causes severe, knife-like pain that is
unimaginable to most of us and results in these patients being
stigmatized and marginalized by doctors and health care providers, who
are frustrated by an inability to help these long-suffering patients.
Total pancreatectomy with transplantation of the patients' own
insulin-producing cells offers patients the chance to remove the source
of the pain and at the same time prevent the side-effects of brittle
diabetes.”
 “What drew me to
this field is the need to take care of these patients who are in so
much pain.” Dr. David Adams “What drew me to
this field is the need to take care of these patients who are in so
much pain.” Dr. David Adams
Adams, chief of the Division of Gastrointestinal and Laparoscopic
Surgery,
said he’s seen the condition reduce war-toughened veterans to tears. He
recalls a patient who had suffered having his jeep blown up in Vietnam,
but said that his pancreatic pain topped that experience to the point
he couldn’t move to even turn around. He related how he had gone to
emergency rooms in intense pain and the staff would think he had just
come in for drugs.
Adams often sees patients after they’ve been referred through the
system by health professionals who don’t know what to do to help them.
The five-year survival rate for patients with chronic pancreatitis is
25 percent.
“What drew me to this field is the need to take care of these patients
who are in so much pain. They’ve always been shunned in the past. You
can’t cure everybody, but you can care for them—always.”
 Dr. Katherine Morgan Dr. Katherine Morgan
Katherine Morgan, M.D., a surgeon who also treats these patients,
agrees. It’s gratifying to be able to have had the opportunity to have
such an impact on so many people’s lives, she said. “We have evolved
into a strong, experienced team which enables us to take care of people
most effectively.”
The islet cell transplant procedure is reserved for those patients who
have failed all medical and endoscopic interventions. The goal is to
achieve optimal pain control and improve quality of life, she said.
“We have seen a significant decrease in the need for narcotic
analgesics in most patients, an overall 57 percent reduction in median
daily oral morphine requirements, with about 30 percent of patients
being able to be narcotic free. Most impressively, patients note a
dramatic improvement in quality of life.”
 Research specialist
Kelly Moxley performs sterility testing on the final islet preparation. Research specialist
Kelly Moxley performs sterility testing on the final islet preparation.
One of the key duties of the pancreas is to produce the hormones
insulin and glugagon to metabolize sugars in the blood, a job done by
islet cells in the pancreas. When the pancreas is removed, the body
loses its ability to produce insulin, so diabetes will occur often in
the form of “brittle diabetes” that is very severe and difficult to
control. In the islet cell transplant, the patients own cells are
extracted and infused into their livers with the hope that patients
will be able to remain insulin independent or at least have a less
severe form of insulin-dependent diabetes.
Adams said MUSC has a long history of being a center of excellence for
pancreatic care. He trained under Marion Anderson, M.D., a former
department chairman who was a highly-respected national leader in the
operative treatment of chronic pancreatitis. Another positive
influence is Peter Cotton, M.D., who initiated the Digestive Disease
Center at MUSC in 1994, with a focus on facilitating multidisciplinary
collaboration.
Collaboration is a key factor to success for the islet transplant
program, which receives support from MUSC’s Center for Cellular
Therapy’s (CCT) clean lab, where islet cells are harvested to be
infused back into the patient’s liver by an interventional radiologist.
Michael Nishimura, Ph.D., CCT scientific director, said the lab, the
only one of its kind in the state, is the future of regenerative
medicine because of the sterile environment created by a special
air-handling system that leaves the lab almost particle free. It
prevents spores, dust mites, mold, bacteria, pollen, viruses and other
particles from contaminating what’s being processed.
For example, the lab gets particle counts of 0 to 1 as compared to a
normal room that would have billions, he said. “That’s the environment
required to do these islet isolations. It enables the institution to do
the cutting-edge of medicine, which is regenerative medicine–giving
back people their own cells to treat diseases. Regenerative medicine is
the future of medicine,” he said, citing a few examples.
“In the future, if you have heart disease, we hope to be able to inject
your own cells back into your heart to help it to remodel the heart.
Similarly, if you have joint problems, we hope to inject your cells
into
whatever joint. The goal will be to have your own cells help
participate in your own tissue or organ repair. You need a facility
like the clean cell lab to do that.”
Islet cell transplants are just the beginning of very exciting
research–from treating juvenile diabetes to Alzheimer’s disease – that
eventually will be done in the lab, he said. “It’s waiting for
someone in the scientific community at MUSC to invest the time and
effort.”
Meanwhile, research continues on islet cell transplants.
Adams said MUSC is in the process of evaluating the effectiveness of
islet cell transplantation for the quality of life and pain relief for
patients, but it’s too early to identify long-term outcomes, he said.
Inflammation of the pancreas causes changes resulting in the production
of extra nerve pain stimulators in the nerves around the pancreas.
Another area of interest is how the disease causes a remodeling of the
pain centers in the brain, something that can be hard to reverse, he
said. The goal is to remove the pancreas before it sets up irreversible
brain pathways and to develop better medications that interfere with
those pathways.
Patients with chronic pancreatitis never know when they’re going to end
up in the emergency room with pain and sometimes vomiting because of
these debilitating attacks, he said. He’s excited MUSC will be
continuing its pioneering efforts. “By intervening early in
pancreatic disease, we can return these people to a somewhat normal
life.”
Autologous Islet
Cell Transplant
1. Patient
goes in for surgery to remove the pancreas. An islet cell transplant
can help patients who are suffering from the pain of chronic
pancreatitis.
2. The
pancreas is put on ice and placed in a special fluid.
3. The organ
undergoes a four-to-five hour process in the Center for Cellular
Therapy’s clean lab where specially trained technicians extract
insulin-producing islet cells.
4. The islet
cells go into an IV bag and are infused into the patient during a
procedure done by an interventional radiologist who uses ultrasound to
guide a catheter into the main blood vessel in the liver.
5. The islet
cells are infused into the liver where they are expected to begin
functioning as a miniaturized pancreas, producing and releasing
insulin. About 25 to 40 percent of patients who have islet cell
transplants will not require insulin treatment. For the remaining
patients who are insulin dependent, their diabetes typically is much
more easily managed.
Friday, Feb. 4,
2011
|
|
|






