|
By
Cindy
Abole
Public Relations
In an effort to provide
better health outcomes and lower health care costs, MUSC's Department
of Family Medicine joined an elite rank by becoming a Patient Centered
Medical Home (PCMH).
Bill Hueston, M.D.,
professor and chairman, Department of Family Medicine, said the model's
multidisciplinary approach offers better, more interactive health care.
This past spring, MUSC Family Medicine achieved a level 3 (the highest
designation) PCMH rating by the National Committee for Quality
Assurance (NCQA) utilizing the Physician Practice Connections program.
The PCMH program evaluates
practices, tools and systems to certify that they meet the NCQA
standards for ensuring that children, youth and adults receive
comprehensive primary care services.
 Family Medicine director Dr. Bill
Hueston, left, reviews a patient's chart with third-year medical
student Guillermo Rivell at the MUSC Family Medicine Center in downtown
Charleston. Left photo: Apothecary show globes, right, grace the counter at
MUSC Family Medicine Center's pharmacy, a symbol of a return to
old-fashioned values. Family Medicine director Dr. Bill
Hueston, left, reviews a patient's chart with third-year medical
student Guillermo Rivell at the MUSC Family Medicine Center in downtown
Charleston. Left photo: Apothecary show globes, right, grace the counter at
MUSC Family Medicine Center's pharmacy, a symbol of a return to
old-fashioned values. 
"With the complexity of
health care today, it is just as important to coordinate care as it is
to deliver care," Hueston said. "What many patients need is for a
practice to develop systems that are responsible for collecting,
interpreting and sharing patient information that can help coordinate
care among all the patient's providers. Having a system and team who
can do this frees up physicians' time to focus on patients with chronic
disease, their management and care. This is the concept behind the
patient-centered medical home model."
This model embraces a
multidisciplinary team approach by relying on physician assistants,
nurse practitioners, medical assistants and others. It also challenges
programs to invest in information technology, electronic medical
records systems, e-prescription management and same-day scheduling to
transform and modernize family practice medicine, according to Hueston.
Medical information and
results (medications, vitals, lab work and specific etc.) are organized
in a patient's electronic medical record for health care specialists to
access and review at any time. The system not only manages information,
but has proven to improve work flow efficiency, reduce staff workloads
and provide more quality time with patients. Patients and physicians
rely on phone calls and e-mail to communicate using a secure, private
web portal.
"Patients like having an
open access to communicate with their physicians. It's quick, effective
and fits into both the patient and physician's daily schedules,"
Hueston said.
 Immunization
nurse
Stella Seels prepares a vaccination. MUSC Family Medicine Center
provides a full scope of family care services including vaccinations. Immunization
nurse
Stella Seels prepares a vaccination. MUSC Family Medicine Center
provides a full scope of family care services including vaccinations.
This systems-view approach
to health care is of particular interest to Hueston, Peter Carek, M.D.,
professor, Department of Family Medicine Residency Program director,
and Allison McCutcheon, quality coordinator in the Department of Family
Medicine. Both physicians are familiar with early PCMH concepts as was
proposed in the 1980s by pediatricians to help manage vulnerable and
disabled children's medical care, and again in 2000 when industry giant
IBM teamed up with the American Academy of Family Physicians and
American College of Physicians to evaluate the efficacy of the PCMH
model to address rising health care costs.
Hueston, Carek and
McCutcheon feel their department is already ahead of most other primary
care practices in valuing PCMH models through the use of processes and
tools such as ongoing registries, a health maintenance reminder system
and various community-oriented primary care projects. The department's
focus on quality and service has always been a part of Family
Medicine's philosophy of practice.
"Our physicians are
already proactive with patients under their care. They're already aware
of what's going on with their patients long before they arrive for an
appointment," said Carek.
 Pharmacist Laverne Smith, right,
reviews
medication details with patient Marlene Cromwell at the downtown
location. The MUSC Family Medicine Center downtown features a number of
services including a full-service pharmacy. Pharmacist Laverne Smith, right,
reviews
medication details with patient Marlene Cromwell at the downtown
location. The MUSC Family Medicine Center downtown features a number of
services including a full-service pharmacy.
The department's focus on
high quality care extends even to residents who train in the
department. The residency program supports several resident quality
improvement projects where resident-physicians, working in small groups
under the guidance of a faculty mentor, develop a systemwide
intervention project (i.e. diabetes blood sugar management,
hypertension, etc.) to improve upon a clinical problem.
"What's key is that our
residents are given dedicated time to focus on a quality improvement
project that's important to their training," Carek said. "We've giving
our residents the tools and experiences and they're using them."
What's new in family
medicine resident training is integrating PCMH concepts into the
curriculum. By doing this, the program is able to prepare the next
generation of practitioners giving MUSC's family medicine physicians an
edge among other professionals.
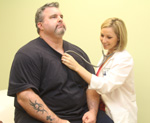 Third-year
family
medicine resident Dr. Emily Bush listens to the heart of patient
Michael Beirne during a recent visit to the University Family Medicine
office in North Charleston. Third-year
family
medicine resident Dr. Emily Bush listens to the heart of patient
Michael Beirne during a recent visit to the University Family Medicine
office in North Charleston.
Family Medicine's road to
success with PCMH is part of a multi-year coordinated effort.
According to Hueston, the
department has done everything needed to prepare for these transitions.
"The future of health care is not just about how much you can do, but
how well you do it. When health care focuses on coordination and
collaboration in care, we can improve quality and outcomes for
patients. I'm hopeful for good change. We all need to work together to
get there."
For information, visit http://www.musc.edu/dfm/.
|



 Family Medicine director Dr. Bill
Hueston, left, reviews a patient's chart with third-year medical
student Guillermo Rivell at the MUSC Family Medicine Center in downtown
Charleston. Left photo: Apothecary show globes, right, grace the counter at
MUSC Family Medicine Center's pharmacy, a symbol of a return to
old-fashioned values.
Family Medicine director Dr. Bill
Hueston, left, reviews a patient's chart with third-year medical
student Guillermo Rivell at the MUSC Family Medicine Center in downtown
Charleston. Left photo: Apothecary show globes, right, grace the counter at
MUSC Family Medicine Center's pharmacy, a symbol of a return to
old-fashioned values. 
 Immunization
nurse
Stella Seels prepares a vaccination. MUSC Family Medicine Center
provides a full scope of family care services including vaccinations.
Immunization
nurse
Stella Seels prepares a vaccination. MUSC Family Medicine Center
provides a full scope of family care services including vaccinations. Pharmacist Laverne Smith, right,
reviews
medication details with patient Marlene Cromwell at the downtown
location. The MUSC Family Medicine Center downtown features a number of
services including a full-service pharmacy.
Pharmacist Laverne Smith, right,
reviews
medication details with patient Marlene Cromwell at the downtown
location. The MUSC Family Medicine Center downtown features a number of
services including a full-service pharmacy. Third-year
family
medicine resident Dr. Emily Bush listens to the heart of patient
Michael Beirne during a recent visit to the University Family Medicine
office in North Charleston.
Third-year
family
medicine resident Dr. Emily Bush listens to the heart of patient
Michael Beirne during a recent visit to the University Family Medicine
office in North Charleston.